Chirurgie bariatrique
Le mode de vie moderne peut être compliqué, surtout lorsqu'il s'agit de bien manger et de vivre sainement. De plus en plus, nous sommes confrontés à des aliments génétiquement modifiés ou à des aliments de restauration rapide avec une nutrition inadéquate et un style de vie occupé et trépidant avec peu d'exercice. Les problèmes suivants, parmi de nombreux problèmes de santé, sont l'obésité comme le diabète, l'hypertension, les maladies coronariennes et l'hypercholestérolémie.
L'IMC ou indice de masse corporelle est une indication de l'obésité, calculée à partir du poids et de la taille afin de déterminer l'équilibre entre le poids et la taille. L'IMC peut être calculé par le poids corporel (kg) divisé par le carré de leur taille (m), les résultats peuvent être interprétés comme suit.
- Insuffisance pondérale : moins de 18,5 (<18,5).
- Idéal : supérieur ou égal à 18,5 mais inférieur à 25 (≥18,5 mais <25).
- Surpoids : supérieur ou égal à 25 mais inférieur à 30 (≥25 mais <30).
- Obèse : supérieur ou égal à 30 mais inférieur à 40 (≥30 mais <40).
- Risque : supérieur ou égal à 40 (≥40).
(https://en.wikipedia.org/wiki/Body_mass_index)
Cliquez pour calculer votre IMC
Lignes directrices pour traiter l'obésité :
1. Plans de régime et exercice
2. Traitement médicamenteux
3. Chirurgie
Plans de régime et exercice
Pour traiter efficacement et en toute sécurité l'obésité, un régime alimentaire sain, faible en glucides et en sucre doit être intégré au mode de vie du patient, ainsi que des séances d'exercice au moins 4 fois par semaine. Pour obtenir le résultat souhaité, chaque séance d'exercice doit également inclure au moins 30 minutes d'entraînement cardio, c'est-à-dire courir, faire du vélo ou nager, car cela aide à brûler les graisses. Si votre IMC est supérieur à 30 et que vous présentez des facteurs de risque, veuillez consulter votre médecin.
Traitement avec des médicaments
Pour les personnes dont l'IMC est supérieur ou égal à 30, un traitement médicamenteux peut être administré sous la surveillance étroite d'un médecin spécialiste. Ce plan de traitement convient également aux personnes ayant un IMC de 27 ou plus avec des facteurs de risque impliqués.
Chirurgie bariatrique :
1. Manchon gastrique (Sleeve Gastrectomie)
Procédure :
Aujourd'hui, la sleeve gastrectomie est l'option de chirurgie bariatrique qui connaît la croissance la plus rapide en Amérique du Nord et en Asie. Dans de nombreux cas, mais pas tous, la sleeve gastrectomie est aussi efficace que le pontage gastrique, y compris les avantages indépendants du poids sur l'homéostasie du glucose. Le ou les mécanismes précis qui produisent ces avantages ne sont cependant pas connus.
(https://en.wikipedia.org/wiki/Gastric_bypass_surgery)
Avantages : C'est la meilleure façon de perdre du poids. Le diabète, les maladies cardiaques, l'hypertension artérielle et l'hypercholestérolémie pourraient également être guéris avec cette procédure.
Inconvénients : Des carences en calcium, en fer et en vitamines peuvent survenir. Il existe un risque d'érosion osseuse et d'anémie.
À Kamol Cosmetic Hospital, nous utilisons la chirurgie mini-invasive ou la laparoscopie qui ne provoque que de petites lésions sur l'abdomen.
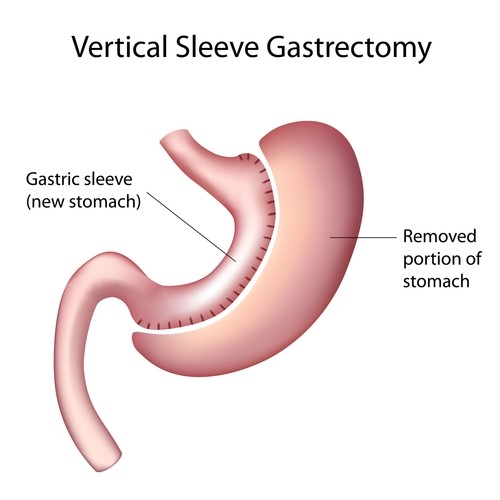
Figure 1 : La gastrectomie verticale en manchon
http://www.nuffieldhealth.com/treatments/sleeve-gastrectomy
Préparation à la chirurgie :
Une liste de spécialistes à consulter avant la chirurgie
1. Les nutritionnistes
Ils peuvent mettre en place de nouveaux plans de régime et déterminer la quantité de nourriture que le patient doit consommer après la chirurgie et comment perdre du poids avant la chirurgie
2. Les psychologues
Aide à gérer et à réduire le stress avant et après la chirurgie
3. Les médecins spécialisés en obésité
Les docteurs en médecine surveillent de près l'état de santé du patient. Ils peuvent offrir des conseils ou des médicaments pour perdre du poids avant la chirurgie.
4. Les chirurgiens experts effectuant des chirurgies sur des patients obèses
La chirurgie peut être pratiquée dans des cas particuliers. Cependant, cette chirurgie présente des avantages et des inconvénients et le patient a le droit de se renseigner avant de décider de subir la chirurgie.
Pour consultation et pratique avec
- La thérapie nutritionnelle pour expliquer combien le client doit manger après la chirurgie. Et comment perdre du poids avant la chirurgie.
- Les psychologues aident à réduire le stress qui peut être plus dans l'avant - après la chirurgie.
- Les docteurs en médecine doivent surveiller la thérapie de conseil en santé. Conseils ou médicaments pour perdre du poids avant la chirurgie.
- L'alternative médico-chirurgicale pour les patients, celle-ci décrit chaque procédures en y énonçant les avantages et las inconvénients de chacune d’entre elle afin que le patient comprennent bien ce que cela implique.
Complications :
- Saignement
- Infections
- Voie d'éjection (déchirures dans les intestins)
- Chirurgies de suivi ou correctives
Les complications post-opératoires peuvent inclure des caillots sanguins provenant d'une maladie pulmonaire, d'une pneumonie ou d'une infection des voies urinaires, qui sont similaires à toute intervention chirurgicale. Cependant, les complications peuvent moins survenir si la chirurgie est pratiquée dans un hôpital ou un centre médical avec une équipe de médecins experts, en particulier des anesthésistes spécialisés dans la prise en charge des patients obèses. Après la chirurgie, un équipement et des soins appropriés doivent être fournis pour surveiller le patient, y compris des équipes d'infirmières et des soignants spécialement formés.
Pourquoi la chirurgie bariatrique est-elle bonne ?
Avec moins de poids et d'obésité, une personne encours moins de risques pour sa santé, notamment le diabète, l'hypertension, les maladies cardiaques, le cancer, l'apnée du sommeil, entre autres. De plus, les personnes moins obèses nécessitent moins de dépenses pour prendre soin de leur santé.
Que se passe-t-il après la chirurgie ?
- Les patients doivent être hospitalisés pendant trois jours pour s'assurer qu'il n'y a pas de complications et qu'ils peuvent fonctionner sans prendre d'analgésique.
- Faites de l'exercice dès que vous vous sentez mieux avec un programme d'exercices spécialement conçu pour vous.
- Adoptez un nouveau régime alimentaire conçu par un nutritionniste pendant au moins un mois.
2. Ballon Gastrique
Le ballon gastrique est une solution efficace contre l'obésité sévère. Il est recommandé aux patients qui ont besoin de perdre du poids avant de subir une opération d'amaigrissement afin de réduire leur risque chirurgical.
Un ballon dégonflé est placé à l’intérieur de la bouche et de l'œsophage, puis rempli de liquide, qui est conçu pour remplir partiellement votre estomac, vous donnant une sensation de satiété. Cela vous aidera à changer vos habitudes alimentaires, à réduire le volume de nourriture consommée et à vous sentir rassasié plus rapidement. Le ballon est conçu pour rester en place pendant un maximum de six mois, après quoi il doit être retiré de la même manière qu'il a été inséré.
Comment le ballon est-il inséré ?
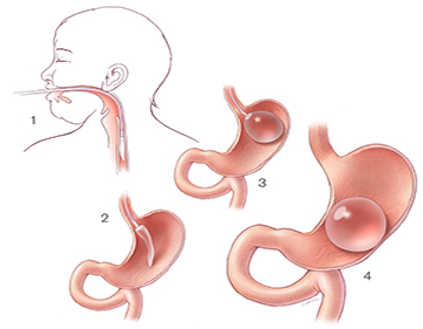
Figure 2 : Les procédures de ballon gastrique
(Ref: www.loyolamedicine.org/weight-loss-bariatrics/gastric-balloon)
Dans la salle de traitement, votre gorge sera aspergée d'un spray anesthésiant. Il a un goût désagréable mais il est très efficace et en quelques secondes, votre gorge sera engourdie. Bien que ce soit une sensation assez étrange, elle est inoffensive et vous aidera à tolérer le tube de gastroscopie (caméra). Si vous avez de fausses dents, vous devrez les retirer. Vous pouvez également avoir une injection pour vous endormir si vous le souhaitez, mais cela sera discuté avec vous.
Une fois que l'infirmière vous a installé confortablement sur le chariot, un protège-dents en plastique sera placé entre vos dents et vos gencives pour garder votre bouche légèrement ouverte. Tout au long de la procédure, votre pouls, votre tension artérielle, votre respiration et vos niveaux d'oxygène seront surveillés, et une petite éponge peut être placée dans une narine pour vous fournir un peu d'oxygène. C'est complètement routinier et il n'y a rien à craindre.
Un endoscope sera ensuite introduit dans votre bouche et descendra dans votre estomac. Cela ne vous causera aucune douleur et n'interférera pas avec votre respiration. Afin d'avoir une vue claire de votre estomac, il peut être nécessaire de mettre de l'air dans l'endoscope. Cela peut vous donner l'impression de vouloir éructer. Une fois l'endoscope retiré, le chirurgien passera le ballon dégonflé dans votre bouche et dans votre estomac. L'endoscope sera réintroduit pour vérifier que le ballon est dans la bonne position avant qu'il ne soit gonflé de liquide.
Régime alimentaire avant la procédure
Avant l'insertion du ballon gastrique, vous devez être à jeûne pendant 12 heures. Lorsque le ballon gastrique doit être retiré, vous devez commencer un régime uniquement liquidien 48 heures à l'avance. Cela signifie, pas de nourriture solide du tout. À ce stade, il peut être utile d'avoir des boissons gazeuses, car elles peuvent aider à nettoyer le ballon, ce qui facilite son retrait. 12 heures avant le retrait du ballon, vous devez être également à jeûne.
Quel régime vais-je suivre une fois le ballon inséré ?
Pendant la première semaine, vous devrez suivre un régime uniquement liquide. Cela permet à l'estomac de s'habituer au ballon. Vous devez boire beaucoup de liquide pour éviter la déshydratation.
Les points clés sont :
• Buvez lentement, sirotez des boissons
• Ne buvez pas plus de 100 ml à la fois
• Buvez environ 2 litres (8 tasses) par jour.
Les meilleurs liquides sont les variétés faibles en gras ou en sucre. Il s'agit notamment du lait demi-écrémé ou écrémé, des yaourts à boire faibles en gras, de la soupe sans grumeaux. Vous devez éviter le café et les boissons gazeuses.
Au cours de la semaine suivante, vous passerez à un régime en purée, suivi d'un régime doux et pâteux, pour finalement passer à un régime normal. Vous verrez la diététicienne une semaine après l'insertion du ballon pour discuter des étapes. De plus, lors de ce rendez-vous, votre plan à long terme sera discuté.
Si vous souffrez de diabète, vous devrez peut-être surveiller et enregistrer de très près votre glycémie, car un changement de votre médication peut être nécessaire.
Quels sont les avantages d'avoir un ballon gastrique ?
La plupart des gens ont peu de problèmes pendant et après la procédure. Cependant, il peut parfois y avoir des complications ou des difficultés telles que :
• Diabète
• Hypertension artérielle
• Cardiopathie
• Douleur articulaire
• Taux de cholestérol élevé
Quels sont les risques et les complications ?
La plupart des gens ont peu de problèmes pendant et après la procédure. Cependant, il peut parfois y avoir des complications ou des difficultés telles que :
• Saignement ou perforation résultant d'une blessure lors de l'insertion ou du retrait du ballon, nécessitant une correction chirurgicale.
• Faibles niveaux d'oxygène dans le sang ou rythme cardiaque irrégulier (ceci est parfois suffisamment grave pour provoquer une crise cardiaque). Afin que nous puissions surveiller ces problèmes, votre niveau d'oxygène et votre pouls seront surveillés tout au long de la procédure.
• Il existe un léger risque pour les dents couronnées ou les bridges. Le risque peut être réduit en nous disant si vous avez l'un ou l'autre de ces éléments.
• Obstruction intestinale par le ballon, lorsqu'un ballon partiellement dégonflé passe dans l'intestin grêle. Ceci est extrêmement rare, mais si cela se produit, il doit être retiré lors d'une opération ou par une procédure endoscopique.
• Un colorant bleu est ajouté à la solution saline qui est injectée dans le ballon, de sorte que dans le cas rare où le ballon devait fuir, vous le sachiez immédiatement par le changement de couleur de votre urine. Si cela devait se produire, vous devez contacter immédiatement l'hôpital afin que le ballon puisse être retiré en toute sécurité.
• Les malaises gastriques, les nausées et les vomissements sont fréquents pendant la première semaine suivant la mise en place du ballon, mais ils persistent rarement après cette période.
• Sensation de lourdeur dans l'abdomen, ou douleur abdominale ou dorsale
• Reflux acide et indigestion (on vous prescrira des médicaments pour réduire votre production d'acide gastrique pendant que le ballon est en place)
• Très rarement, les patients développent une infection pulmonaire après la procédure. Si vous développez une toux, vous devez contacter votre médecin.
La probabilité que ces risques se produisent est faible, mais il est important que vous en soyez conscient et que vous disposiez de toutes les informations nécessaires avant d'accepter la procédure.
Que se passe-t-il avant la procédure ?
Si la procédure de ballon gastrique est une option sûre et appropriée pour vous, il vous sera demandé de vous rendre à l'hôpital pour une évaluation préalable à la procédure. Lors de ce rendez-vous, nous vous poserons des questions sur vos antécédents médicaux, vos médicaments et toute autre opération que vous avez pu avoir dans le passé. Vous devrez peut-être subir des tests de routine, par exemple un tracé cardiaque (ECG), une radiographie et des tests sanguins.
Que se passe-t-il à l'admission à l'hôpital ?
Sauf indication contraire, vous viendrez à l'hôpital le matin de votre intervention. Lors de l'admission, les médecins et les infirmières répondront à toute autre question que vous pourriez avoir. Une infirmière vérifiera qu'il n'y a pas eu de changements significatifs dans votre état de santé depuis votre pré-évaluation, et votre température, votre pouls, votre tension artérielle et votre respiration seront tous enregistrés. Avant d'avoir votre procédure, il vous sera demandé de mettre une blouse. Il vous sera également demandé de porter des bas de contention (antiembolique). Ils favorisent la circulation sanguine dans les veines profondes des jambes et réduisent ainsi le risque de formation de caillots sanguins. Vous devrez les porter pendant environ six semaines après votre intervention. Il vous sera demandé de marcher jusqu'à la salle d'intervention.
Vais-je être endormi ?
Un spray anesthésiant pour la gorge sera utilisé avant la procédure. Alternativement, vous pouvez recevoir des médicaments dans un tube dans votre bras ou votre main, ce qui vous rendra très somnolent. Vous devriez toujours être en mesure d'entendre ce qui se dit et de coopérer avec les instructions verbales, mais plus tard, vous n'aurez peut-être que peu ou pas de souvenir de la procédure.
À quoi puis-je m'attendre après la procédure ?
De la salle d'intervention, vous serez transféré au service de réveil. Le personnel infirmier vérifiera votre pouls, votre tension artérielle, votre température et votre respiration. Vous pouvez avoir mal à la gorge à cause de l'équipement endoscopique. Si vous avez reçu une sédation, vous pouvez vous sentir somnolent pendant un certain temps et vous pouvez recevoir de l'oxygène par deux petites pinces dans votre nez jusqu'à ce que vous soyez complètement réveillé. Vous serez encouragé à vous lever et à vous déplacer peu de temps après votre intervention. Ceci afin de réduire le risque de développer un caillot sanguin.
Vais-je me sentir malade ?
De nombreuses personnes se sentent malades et vomissent après la procédure et pendant un certain temps après. On vous prescrira des médicaments contre la nausée, qui sont des médicaments qui aident à soulager les nausées et les vomissements. Le malaise devrait s'estomper une fois que votre estomac se sera habitué à la présence du ballon.
Aurai-je mal ?
Vous pouvez avoir une sensation de lourdeur dans l'abdomen ainsi que des douleurs le dos et l’abdomen. Des analgésiques vous seront prescrits pour aider à soulager cela.
Quand pourrai-je rentrer chez moi ?
Vous pourrez généralement rentrer chez vous le jour ou le lendemain de votre intervention, selon ce que vous ressentez. Vous devez avoir quelqu'un responsable pour vous ramener à la maison car vous ressentirez peut-être encore les effets de la sédation. Nous conseillons également que quelqu'un reste avec vous pendant 24 heures.
Quels seront les soins de suivi ?
Vous recevrez un rendez-vous avec la diététicienne et l'infirmière spécialisée du service de consultation externe environ une semaine après votre retour à la maison. Vous recevrez également les numéros de téléphone de l'infirmière spécialisée et de la diététicienne à contacter pour tout conseil dont vous pourriez avoir besoin à d'autres moments. Lorsque votre ballon est prêt à être retiré, six mois après la mise en place, l'hôpital organisera son retrait et vous enverra un rendez-vous.
Ref: Doncaster and Bassetlaw Hospitals NHS Foundation Trust. (2012). Gastric Balloon procedures. Bariatric surgery
Apprendre à connaître la chirurgie bariatrique
Régime de gastrectomie à manches
La gastrectomie à manches est un type de chirurgie bariatrique qui consiste à réduire la taille de l'estomac
Gastrectomie à manches VS Pontage gastrique
L'obésité est un problème croissant dans le monde entier et la chirurgie bariatrique est devenue une option de plus en plus populaire
Quels sont les effets secondaires de la sleeve gastrectomie ?
La sleeve gastrectomie est une chirurgie de perte de poids populaire qui consiste à retirer une grande partie de l'estomac pour réduire sa taille et sa capacité à se nourrir.
Avis sur la gastrectomie à manches
Pourquoi la sleeve gastrectomie est-elle envisagée pour perdre du poids ?
La gastrectomie en manchon, également connue sous le nom de gastrectomie en manchon vertical, est une chirurgie de perte de poids qui consiste à enlever une grande partie de l'estomac, laissant un estomac plus petit en forme de "manchon". Cet estomac plus petit peut contenir moins de nourriture et, par conséquent, les patients se sentent rassasiés plus rapidement et mangent moins. La procédure est généralement réalisée par laparoscopie, qui est moins invasive que la chirurgie ouverte et a un temps de récupération plus rapide.
L'un des principaux avantages de la sleeve gastrectomie est qu'elle peut entraîner une perte de poids importante. En moyenne, les patients peuvent s'attendre à perdre 50 à 70 % de leur excès de poids au cours de la première année suivant la chirurgie. La perte de poids a également tendance à être plus stable et plus durable que d'autres options de perte de poids telles que le régime alimentaire et l'exercice.
La sleeve gastrectomie entraîne également des changements hormonaux qui favorisent la perte de poids. La ghréline, connue sous le nom d’ « hormone de la faim », est produite dans l'estomac. Les niveaux de ghréline diminuent après la sleeve gastrectomie, entraînant une réduction de la faim et des fringales.
Bien que la sleeve gastrectomie soit considérée comme moins invasive et présente un risque de complications moindre par rapport à d'autres chirurgies de perte de poids telles que le pontage gastrique, il s'agit toujours d'une chirurgie majeure et doit être abordée avec prudence. Comme pour toute intervention chirurgicale, il existe des risques tels que des saignements, des infections et des caillots sanguins.
Il est important de noter que la chirurgie bariatrique doit être considérée comme un dernier recours après que toutes les autres options ont été épuisées. Les patients doivent également être sous la surveillance étroite d'un professionnel de la santé et subir une évaluation complète avant de subir une intervention chirurgicale pour s'assurer qu'ils sont des candidats appropriés. De plus, les patients devront apporter des changements importants à leur mode de vie, notamment des exercices réguliers, une alimentation saine et un suivi avec leur équipe médicale pour garantir les meilleurs résultats.